study overview
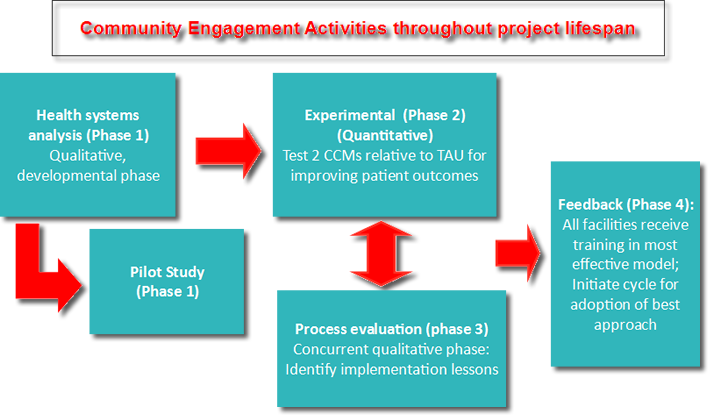
Hover over the Phases to view more information
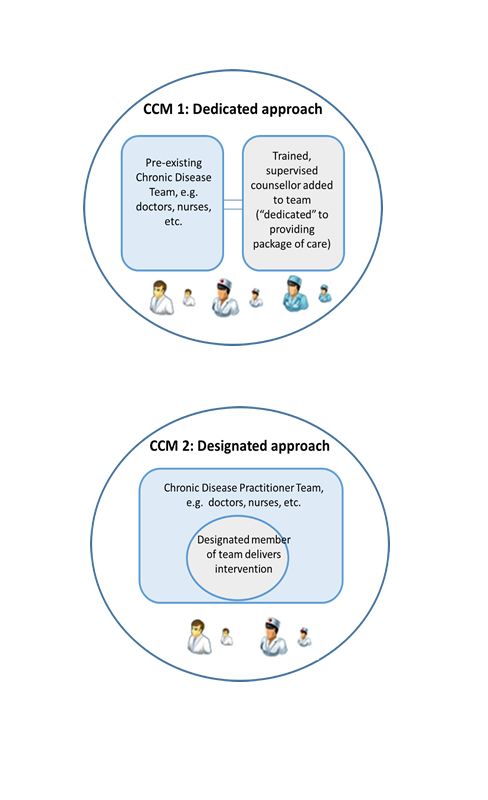
Collaborative Care Model 1: Dedicated approach
In clinics assigned to this approach, we will provide the chronic disease team with basic training in common mental disorders and prepare them to integrate a brief intervention for common mental disorders into chronic disease care. This brief counselling intervention will be provided by a trained Community Health Worker (CHW). We will add an additional CHW to the existing chronic disease team. This person will be dedicated to providing the counselling programme across both HIV and diabetic clinics.
The brief counselling programme provided by the CHW consists of three structured counselling sessions based on a blend of motivational interviewing and problem solving therapy (MI-PST). Supervision, debriefing, and ongoing training will be provided to the CHW to support the delivery of a quality service.
Collaborative Care Model 2: Designated approach
In this approach, we also will provide the chronic disease team with basic training in common mental disorders and prepare them to integrate a brief intervention for common mental disorders into chronic disease care. Unlike the dedicated approach, in the designated model we will identify CHWs already working as adherence counsellors within primary care facilities who will be designated to provide the counselling programme across both HIV and diabetic clinics in addition to their usual adherence counselling responsibilities.
CHWs in the Designated approach will be trained to provide exactly the same structured counselling programme as provided in the Dedicated model. They will also receive the same amount of supervision, debriefing, and ongoing training as provided to CHWs in clinics assigned to the dedicated approach.
Treatment as usual (TAU)
In clinics assigned to Treatment as Usual, patients will receive the types of services that are normally offered to patients with chronic diseases and a suspected common mental disorder (such as depression, anxiety or alcohol-related problems). Generally, if a health care provider suspects that a patient may have a common mental disorder, the patient would be referred to a mental health nurse for further assessment and referral, an off-site organization providing mental health services or a social worker. In addition to this referral, we will provide patients with an information brochure that provides contacts for mental health and substance use services.